PLoS ONE Publishes its 20,000th Manuscript!
Today we are happy to announce that PLoS ONE has published its 20,000th manuscript! We could not have gotten here today without the help and support of our authors, reviewers, academic editors, and the OA community. Thank you for helping us to achieve this incredible milestone!
To mark this occasion, we’ve asked Dr. Brian Oliver and Dr. Stephen Liggett, authors of the 20,000th manuscript, b2-Agonist Induced cAMP Is Decreased in Asthmatic Airway Smooth Muscle Due to Increased PDE4D to tell us a bit about their article, their background, and their research via email.
To begin, give us a summary of your research?
BO: In our research, we have been examining how the drugs, which relax bronchial air passages of people with asthma, work. These therapies bind to, and activate the ß2 receptor. This receptor induces the formation of cAMP, which initiates muscle relaxation. In turn cAMP is regulated by an enzyme phosphodiesterase 4 (PDE4D). We have discovered that airway smooth muscle cells from people with asthma have increased phosphodiesterase 4. As phosphodiesterase 4 degrades cAMP, our research has important implications for the treatment of asthma.
SL: We found that airway smooth muscle cells derived from asthmatics are “hard-wired” to have a defect in signaling by the beta-2 adrenergic receptor. This defect is an enhanced phosphodiesterase activity, essentially leading to rapid metabolism of intracellular cAMP, rendering the asthmatic smooth muscle cell with a depressed response to beta-agonists. Beta-agonists are the major drugs used to relax airway smooth muscle and open airways in asthma. The hard-wiring part is quite intriguing. It has been generally thought that inflammation in asthma leads to signaling defects, at both the relaxation side (such as with beta-2 adrenergic receptors) and the exaggerated bronchoconstrictive receptors such as the M3 muscarinic receptor. However, these cells were kept in cell culture media and passaged multiple times, and obviously removed from the inflammatory environment in the asthmatic patients. So, this is either a genetic or epigenetic effect.
When did you become interested in studying asthma?
BO: Before starting my PhD, I realized that asthma is a disease which effects a large proportion of the population (at least 10%), and is also a disease in which there is a need to develop better therapeutics. I was fortunate to be employed at the National Heart and Lung Institute,UK where I examined basic science mechanisms underpinning asthma, and I realized that this is where my future career would be. I then travelled to Australia to undertake my PhD with Professor Judith Black who is one of the leading experts in airway smooth muscle biology, and as they say I have never looked back.
SL: I was a post doc at the HHMI with Robert Lefkowitz during the cloning and initial characterization of the adrenergic receptors, and my lab studies basic structure/function relationships. But I have always been drawn to the translational aspect of understanding how G-protein coupled receptor signaling is so aberrant in asthma. And, I have persistent asthma myself, so there is a personal interest in further understanding these issues. Actually, I am wondering if this has been a driving force for longer than I might realize. I got irritated that we knew so little about human rhinoviruses (a major cause of asthma exacerbations), so we just sequenced every known common cold strain to get a handle on that. And we have made dozens of transgenic mice aimed at understanding smooth muscle signaling, all pointing towards asthma. So as it was with this study, we went against some old dogma and just pushed on. Studying human cells derived from affected and unaffected individuals is hard, but it must be done if we are to crack this nut.
Your manuscript has several figures in it. Which one do you think is the most important for people to pay attention too?
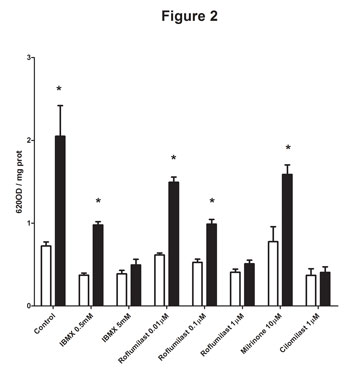
BO: Figure one represents the initial finding which led to this study, however this for me is not the most important figure. Figure two is. In figure two we measured phosphodiesterase activity in asthmatic airway smooth muscle cells, and found increased activity in the asthmatic cells. To investigate which phosphodiesterase was increased we used a series of phamalogical inhibitors and were able to demonstrate that PDE4 activity was specifically increased in the asthmatic cells.
During the course of your research for this paper, did you find anything unexpected?
BO: Our initial finding was that ß2 agonist induced cAMP was lower in the asthmatic cells. There are several reasons described in the literature as to why this could occur. However increased PDE4 activity was not one of these.
SL: The hard-wiring aspect, and where the defect was. I figured that it would be upstream of adenylyl cyclase.
What’s next? Where would you like to go from here?
BO: In asthma, virus infection precipitates exacerbations (bronchial contraction) in which ß2 agonist don’t work as well as they do at other times. As we have now shown that PDE4 activity is increased in asthma we want to investigate the role of PDE4 in virus-induced exacerbations.
SL: Now that we have this identified, we would like to devise a “workaround” strategy, that will allow for effective bronchial dilatation by beta-agonists (or another receptor), so as to provide more effective treatments.
What made you decide to submit to PLoS ONE?
BO: There are several factors to consider when submitting a paper to a journal. Amongst the most important are: journal prestige, length of review process, and the accessibility of the paper post publication. PLoS ONE is a good journal by all measures, and based upon our previous experience we knew that we would receive a quick and fair review. Also, being open access allows anyone with internet access to see our paper and, as such, allows us as scientists to share our findings with the world.
SL: The general readership is a big plus. As we all know so well, these pathways and proteins are in many cell types and we wanted investigators from many fields to be aware of what we found, so that there can be more “collective thinking.”